Introduction
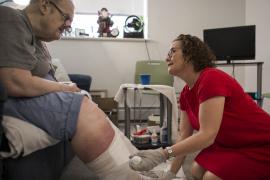
Maria Viera, age 75, takes a dozen medications to treat her diabetes, high blood pressure, mild congestive heart failure, and arthritis. After she begins to have trouble remembering to take her pills, she and her husband visit her primary care physician to discuss this and a list of other worrisome developments, including hip and knee pain, dizziness, low blood sugar, and a recent fall. Maria’s primary care doctor spends as much time with her as he dares, knowing that every extra minute will put him further behind schedule. Yet despite his efforts, there is not enough time to address her myriad ailments. She sees several specialists, but no one talks to all her providers about her care, which means she may now be dealing with conflicting recommendations for treatment, or medications that could interact harmfully. As a result, Maria is at high risk for avoidable complications and potentially preventable emergency department visits and hospital stays.
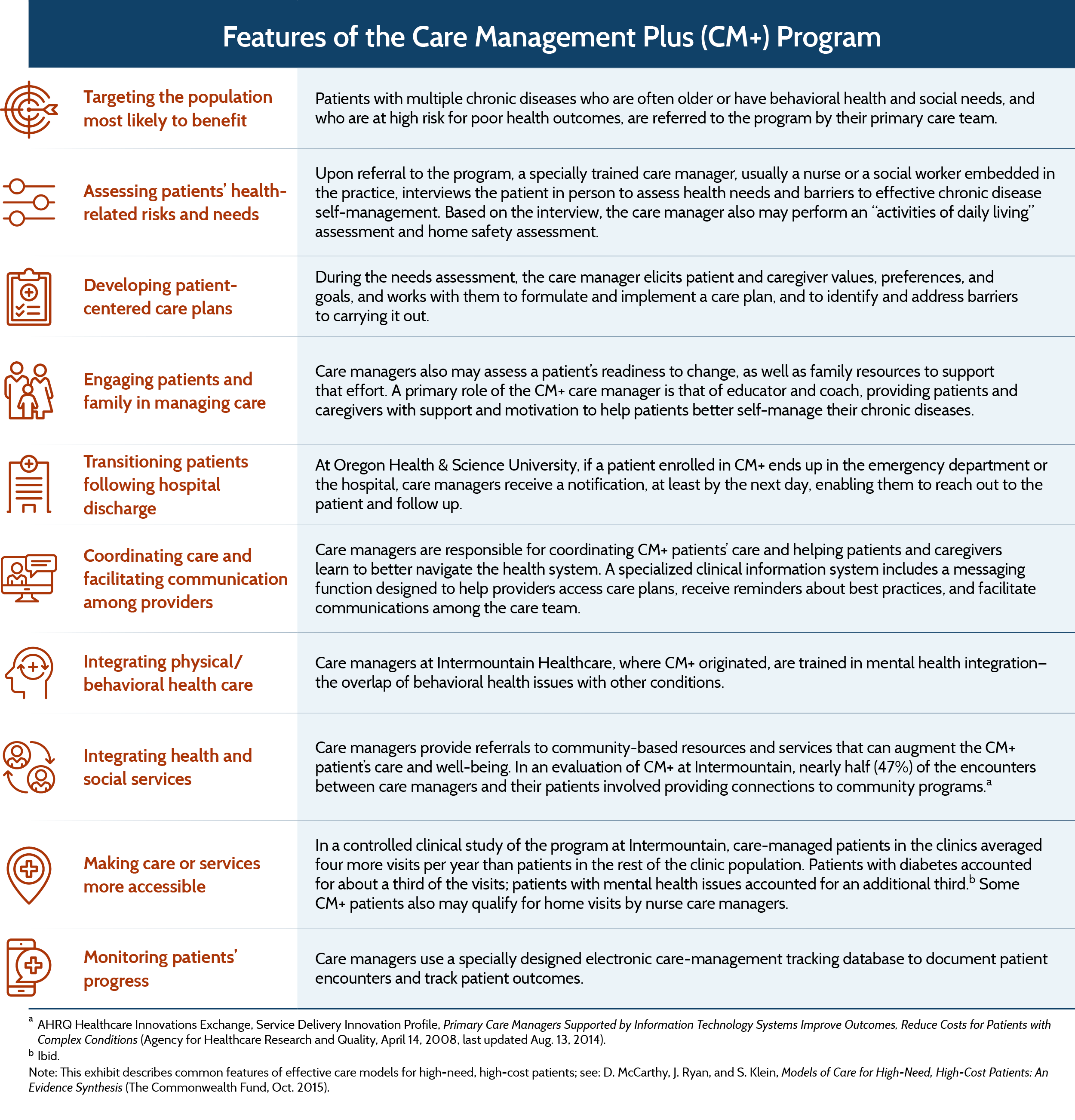
Maria is a “persona” created by David A. Dorr, M.D., to illustrate the type of patient who might benefit from Care Management Plus, a health care delivery model designed for older adults with multiple chronic conditions. Dorr and colleagues at Intermountain Healthcare, an integrated care delivery system serving patients in Utah and Idaho, created the program some 15 years ago not only to improve the quality and coordination of care but also to reduce health care costs and support primary care providers who treat these high-need, high-cost patients. Care Management Plus is built on the pillars of the Chronic Care Model, which identifies six essential components for high-quality chronic disease care: the community, the health system, self-management support, delivery system design, decision support, and clinical information systems.1
Care Management Plus itself has roots stretching to 1995, when Intermountain extended its hospital-based care-management program to 10 primary care clinics within its Medical Group, which employs primary care physicians and specialists to provide care to Intermountain patients in clinic settings. The clinics hired “continuum care managers,” with an initial focus on improving diabetes management and thereby reducing avoidable hospitalizations, unnecessary primary care use, and costs. In 2001, the John A. Hartford Foundation’s Geriatric Interdisciplinary Teams in Practice initiative provided support for Intermountain to expand the focus of this work by adding training and specially designed information technology tools. The continuum care managers helped develop these tools, aiming to better address the medical, mental health, and social needs of older patients with multiple chronic conditions.
Between 2002 and 2005, the program was tested in seven primary care clinics within Intermountain, where physicians were given the option to refer chronically ill patients age 65 and older to an on-site nurse care manager. At the end of two years, patients enrolled in Care Management Plus, especially those with diabetes, had fewer hospitalizations and lower mortality compared with matched controls (see “Results”). The program had a positive effect on physicians as well. Doctors in the intervention clinics who were “high users” of the program — meaning they referred more than 2 percent of their patient population to a care manager — increased their productivity and were more satisfied.2
With the demonstration of these benefits, the Hartford Foundation in 2006 awarded Dorr and Cherie P. Brunker, M.D., the chief of geriatrics at Intermountain, financial support to disseminate the program nationally. The model, branded Care Management Plus, or CM+, has now been implemented in 420 primary care clinics nationwide, covering three million patients. This profile describes the program’s implementation at Intermountain, and at Oregon Health & Science University (OHSU) in Portland, where Dorr joined the faculty in 2005 and is now professor and vice chair of clinical informatics in the Department of Medical Informatics and Clinical Epidemiology.
Population Served
Embedded in primary care clinics, Care Management Plus targets Medicare patients (age 65 or older) and other populations with multiple chronic conditions. As a rule of thumb, about 5 percent to 10 percent of patients in primary care practices using CM+ are invited to participate in the program.
Patients of all ages have been served by the program at Intermountain, which has made care management a standard feature of its “personalized primary care practices” — Intermountain’s version of the patient-centered medical home model. At OHSU, CM+ is used in five large primary care clinics serving two populations: adults ages 40 to 65 with multiple chronic diseases that frequently include diabetes or cardiovascular illness, and are often coupled with behavioral health or substance abuse issues; and older adults who are growing frail or have multiple chronic conditions, and who are at risk of functional decline and may become unable to live independently. Patients entering the program are often in need of a variety of social services, like Supplemental Nutrition Assistance Program (SNAP) benefits.
Patients may be identified for CM+ using risk stratification, disease condition, and algorithms. But referral to the program within Intermountain and OHSU is intentionally flexible and inclusive, with discretion given to the patient’s primary care team.

Care managers like Nancy Swanson, R.N., who works in a large Intermountain internal medicine clinic in Salt Lake City that currently serves about 6,500 adult patients, identify patients for care management in two ways. One way, introduced in the summer of 2016, is through a “high risk” list generated quarterly by the Integrated Care Management division. The list alerts care managers in Intermountain’s primary care clinics if any of their patients are among the health system’s top 1 percent of highest-use, highest-cost patients—or at risk of becoming so. It is these individuals who could potentially benefit the most from care management. The list is created using an algorithm that takes into account numerous factors ranging from patients’ recent use of health care services and costs to their diagnosed chronic conditions and predictive risk of adverse events. “A lot of the folks on the list recently had a major surgery, and I reach out to them to see if I can be of service,” says Swanson, who earlier worked as a surgical nurse and in a GYN oncology clinic. “Some are overjoyed to hear from me, while others will say, ‘I’ve got it all in hand.’”
A patient that needs some extra help may not be high acuity at the time, but if they don’t get an intervention they are going to be.
Patients are also identified via direct referral from providers. In the clinic where Swanson works, these patients range widely in age from their 30s to their 90s, but all tend to have comorbidities and chronic conditions — often uncontrolled diabetes or a mental illness, such as severe depression — that make it difficult for them to take care of their physical health. “A patient that needs some extra help may not be high acuity at the time,” Swanson says, “but if they don’t get an intervention they are going to be.”
Leaders at both institutions strongly encourage care teams to use their clinical intuition and judgment to determine which patients to refer, so that patients who might benefit are not overlooked. “Even the best risk stratification and algorithms have not been able to identify at least 20 percent of people who appear to benefit from care management, and it may be because of an inability to capture psychosocial issues,” says Teresa Garrett, R.N., assistant professor at the University of Utah College of Nursing and formerly assistant vice president for Integrated Care Management at Intermountain.3
Key Features
Care Management Plus Training and Curriculum
Training for CM+ care managers, who are usually nurses or social workers, starts with an intensive one-day, in-person workshop that lays a foundation of knowledge in the core competencies of care management. The workshop is followed by eight weeks of online instruction, hosted by OHSU, including assignments, online discussions, and chats with experts. The training covers patient assessment, motivational interviewing, quality improvement, and the information technology elements of CM+; protocols and patient education for specific chronic diseases, including diabetes, hypertension, asthma, and chronic obstructive pulmonary disease; care for seniors and caregiver support; and ways to connect patients with community resources. Intermountain’s Brunker directs the CM+ training, which, in addition to care managers, draws clinic managers, physician leaders, pharmacists and other members of the care team. Participants can earn continuing education credits for the in-person and online portions.
Embedded Care Managers
Care managers are full-fledged members of the practice’s care team, with office space located in the practice. They are hired by and report to practice managers. Within OHSU’s general internal medicine clinic, a care manager is assigned to each of the six clinical teams, made up of eight to 10 providers; each care manager works with about 200 patients. At Intermountain, each care manager is affiliated with a personalized primary care practice and is responsible for about 250 patients.
Care managers can take the additional time with patients that providers cannot. “A provider in our clinic would always say, ‘Nancy has the gift of time,’” Swanson says. “And I do. I don’t have to rush patients.” Dorr sees the care managers at OHSU as being similarly “gifted” with time. “They are not fee-for-service, churning through 20 or 28 patients a day,” he says.
During the initial visit, the care manager assesses the patient’s needs. A key part of that first encounter is eliciting the patient’s goals and priorities. Based on the information gleaned, the care manager, in partnership with the patient, develops a care plan tailored to that patient. Subsequent encounters may happen face to face or by telephone. The amount of contact varies depending on the patient. During the evaluation of CM+ at the seven clinics within Intermountain, care managers had, on average, 4.3 encounters with a patient, and the average amount of time patients spent in the program was just under four months (112 days).4

Patient and Caregiver Engagement and Empowerment
Care managers establish a trusting relationship with patients and help them identify: health care goals; any barriers that may be holding them back from achieving those goals, such as untreated depression or an exhausted caregiver; and ways to overcome the barriers. They educate patients about their conditions and medications so they can better understand their role in self-management. They also provide connections to community resources and support.
In the evaluation of CM+ at Intermountain, nearly half (47%) of encounters between care managers and patients involved establishing connections to community-based programs. Commonly needed services were those addressing caregiver fatigue, medication assistance, and financial concerns.5 These are still common needs today, says Swanson, who adds that transportation to appointments is another problem area, especially for older patients who no longer drive. A local government agency, Salt Lake County Aging & Adult Services, offers a program in which volunteer drivers take older adults to doctors’ appointments, but Swanson says many patients are not aware it exists. “As a care manager,” she says, “you become an expert in what your community has to offer as far as no-cost or low-cost resources.”
When possible, CM+ seeks to help patients and caregivers help themselves. “Care managers could spend an infinite amount of time with populations like these, so there has got to be a partnership with the patients,” Dorr says. At OHSU, care managers try to draw on a patient’s social support system, asking, “Is there someone in your life who can support you in these changes you are making and be an accountability partner?”
Use of a Specialized Clinical Information System
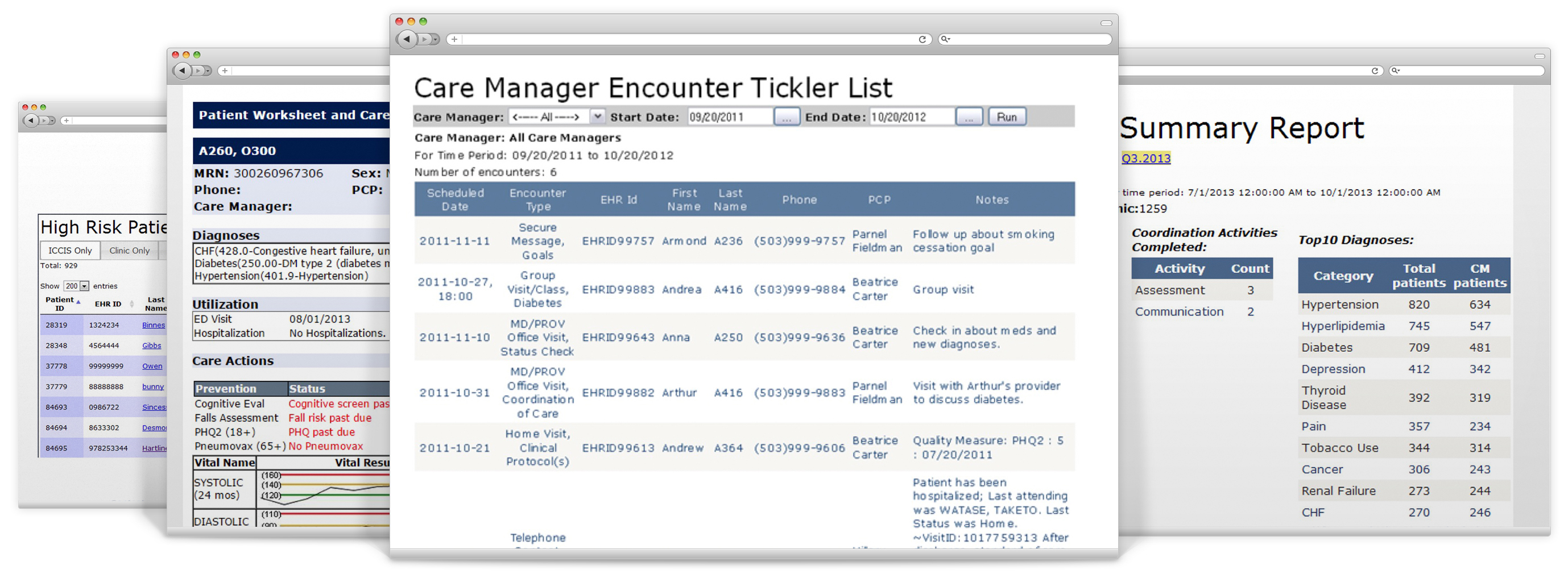
A suite of sophisticated health information technology tools for population management, developed at Intermountain and refined by Dorr and his team at OHSU, supports the work of care managers and the interdisciplinary care team. Known as the Integrated Care Coordination Information System (ICCIS), this web application “sits on top of” a patient’s electronic health record and is adaptable for use with several EHR systems.6 ICCIS allows practices to:
- track patient encounters and record activities
- create “tickler,” or reminder, lists
- perform assessments for depression and functional status (PHQ9 and ADL/IADL questionnaires)
- see, at a glance, in a “Patient Worksheet,” a patient’s chronic conditions, medications, pertinent lab results, and receipt of preventive care, as well as their goals and the results of assessments of depression and functional status, and
- generate clinic summary and quality performance reports.
Financing
In the primary care clinics at OHSU, the estimated salary and training cost for a care manager is $90,000 to $100,000 per year, based on the assumption that the care manager is a senior-level nurse and the practice has eight to 10 providers. A specialized population-management information system to track patients, organize data, and generate performance reports for the primary care clinical team would be an additional cost for clinics that do not already have such a system in place, but most practices at OHSU have this system now. Smaller clinics with just three or four providers have made the model work less expensively by using a medical assistant (MA) as the care manager. “Very small clinics often have a more focused, constantly-in-touch team,” Dorr says, “so the experience of the providers can be more easily shared with the MA.”
Primary care clinics may now be able to leverage alternative payment models such as capitation, per-member, per-month fees, and chronic-care management codes, to help offset the program’s cost. A cost analysis of the program’s implementation at Intermountain in the early 2000s, however, suggested that the program paid for itself through enhanced provider productivity. In the seven primary care clinics at Intermountain where the program was tested, providers who referred patients to a care manager were 8 percent to 12 percent more productive, as measured by relative value units, than providers at 14 control clinics that did not use the program.7 The additional annual revenue generated as a result was estimated to be $99,986 per seven-physician clinic — almost $8,000 above the cost of the salary, training, and other expenses associated with employing a care manager ($92,077).8 Home visits conducted by nurse care managers also can be a source of additional revenue for clinics that adopt CM+. Reimbursements for such visits can bring in an additional $10,000 per year in a seven-physician clinic.9
Since 2001, the Hartford Foundation has provided more than $5 million to develop and disseminate CM+. In November 2011, the Gordon and Betty Moore Foundation awarded OHSU a multiyear, $1.6 million grant to undertake a randomized controlled trial in four diverse health care settings within Oregon, to determine whether an enhanced version of CM+ tailored for the patient-centered medical home environment would lead to improved patient outcomes and lower costs of care. The Agency for Healthcare Research and Quality (AHRQ) and the National Library of Medicine (NLM) also have provided funding for the program.
Results
The controlled clinical trial at Intermountain in the early 2000s found that patients enrolled in CM+ had slightly more emergency department visits but lower annual mortality rates than those in the control group. Patients with diabetes especially benefited: in addition to lower mortality, they had significantly fewer hospitalizations than diabetic patients in the control group (see chart below). The potential savings to Medicare from decreased hospitalizations were estimated at $70,349 per clinic per year for diabetic patients enrolled in the program.10
Insights and Lessons Learned
Hire care managers carefully. The “right” people for the job, according to Dorr, are willing to maintain their relationships with patients and are enthusiastic about helping people cope with complex issues. Personal traits including enthusiasm, adaptability, and the ability to deal with complexity may be among the most important qualifications. Swanson, asked to describe her day-to-day routine, laughs and says, “I joke that when I come through the door in the morning I literally have no idea what I might encounter.”
At the behest of clinics looking to hire care managers, Dorr and his colleagues prepared a job description that includes “positive attitude” and “ability to effect change” among the minimum qualifications. “There are some fluffier-sounding credentials in there, and some clinics will say, ‘I don’t know what that means,’ and just hire someone with a nursing degree,” Dorr says. “Then they get turnover and they get frustrated.”
Practices may need persuading that IT and data are a boon rather than a bane. “A lot of people feel that health information technology is a detriment to their workflow and a pain to deal with,” Dorr says. At some clinics, implementing CM+ means helping providers and clinical staff move from a place where they feel the IT system is painful to a place where they feel comfortable using data regularly. Dorr has observed that the most successful adopters of CM+ are the clinics with the motivation and ability to review data more systematically, and to understand if the changes they are making in their practice have resulted in the improvements they expected.
A 20th-century curriculum may not teach 21st-century skills. It can be challenging to find people trained in population health management and data management, subjects not traditionally a part of nursing or medical school, says Brunker, who, in addition to being the chief of geriatrics at Intermountain, is an associate professor at the University of Utah School of Medicine. As a result, substantial training must often happen in the workplace. In an effort to bridge this education gap, Utah’s higher education system, department of workforce services, and office of economic development convened a work group of Utah health care systems and nursing programs. The group identified opportunities for curricular development in undergraduate nursing programs, and helped to create a new master’s program in nursing, with an emphasis on care management, at the University of Utah College of Nursing.11 Intermountain Healthcare offers clinical sites for the program.
Practices can finally get money directly from payers to cover the costs. With payers including Medicare offering risk-stratified reimbursement for care management, and other payment models emphasizing high-quality care, practices have more opportunities than ever to recoup the costs of implementing a program like CM+. While practices no longer have to await a bump in productivity to begin to offset the program’s costs, the relatively modest ($20 to $40) per-member, per-month fees, more complicated code sets, and payment lags at the outset can still make the transition challenging, especially for smaller practices, which may not see the financial benefits immediately.
Next Steps
Leaders are examining how the principles of the CM+ model can be applied to serve persistently high-use, high-cost patients who may benefit from more intensive care management than can be provided in a primary care clinic setting (see “Adapting the Model”). Garrett, of the University of Utah College of Nursing, says that in a new world of value-based purchasing and alternative payment models, “a sweet spot moving forward is to understand how a comprehensive care-management approach can help patients who have truly complex disease management, social determinants of health, and behavioral health issues be healthier.”